Although ankylosing spondylitis (AS) and related spondyloarthritis (SpA) conditions primarily affect the spine, the disease can influence many other parts of the body. Spondylitis does not follow a predictable pattern, two individuals, even within the same family, may experience very different symptoms. While inflammation of the eye (iritis) is quite common, neurological issues occur rarely, and shoulder involvement falls somewhere between. The chronic pain caused by ongoing inflammation varies widely, ranging from mild discomfort to severe, mobility-limiting symptoms.
People who experience their first symptom of ankylosing spondylitis usually look for help and information by joining communities such as the rheumatoid arthritis support group. The first indications of this condition present themselves in a way which makes them difficult to identify, as they resemble other medical issues. The process of understanding AS enables doctors to distinguish this condition from other related conditions, which includes reactive arthritis that shows identical or comparable symptoms.
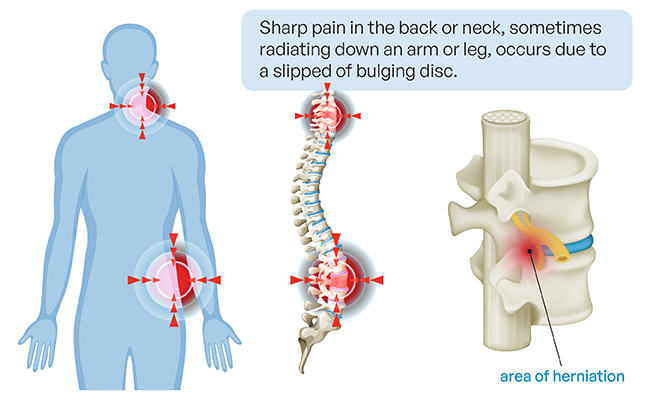
How untreated inflammation can affect the spine, joints, and overall health over time
While Ankylosing Spondylitis has no cure, early and consistent treatment can slow progression and reduce complications.
Key management approaches include:
Many people living with Ankylosing Spondylitis delay medical consultation because early symptoms often resemble common back pain or muscle stiffness. However, early medical evaluation is critical to prevent long-term complications and preserve mobility.
You should consider seeing a doctor preferably a rheumatologist if you experience any of the following signs:

While Ankylosing Spondylitis is a lifelong condition, early diagnosis and proper management can significantly reduce symptom severity. Treatment plans may include medication, physical therapy, posture management, and lifestyle adjustments.
Equally important is emotional and community support knowing you are not alone in this journey.
What’s new in our journey against arthritis and spondylitis.