Psoriatic arthritis (PsA) is a chronic autoimmune disease that causes inflammation of the joints and connective tissues. It primarily occurs in people with psoriasis, a skin condition marked by thick, scaly, red patches. In PsA, the body’s immune system mistakenly attacks healthy tissues, leading to joint pain, swelling, stiffness, and sometimes irreversible joint damage if untreated.
PsA is unique because it affects both the skin and joints and can appear in different forms in different patients. The severity varies widely, some people experience mild discomfort, while others face significant joint damage and disability. Early detection is key: with timely treatment, patients can control symptoms, reduce inflammation, maintain mobility, and prevent long-term damage.
Beyond physical symptoms, PsA can affect emotional well-being. Chronic pain and visible skin lesions may lead to stress, anxiety, or social withdrawal. Support from healthcare providers, family, and patient communities is important for managing the condition effectively.
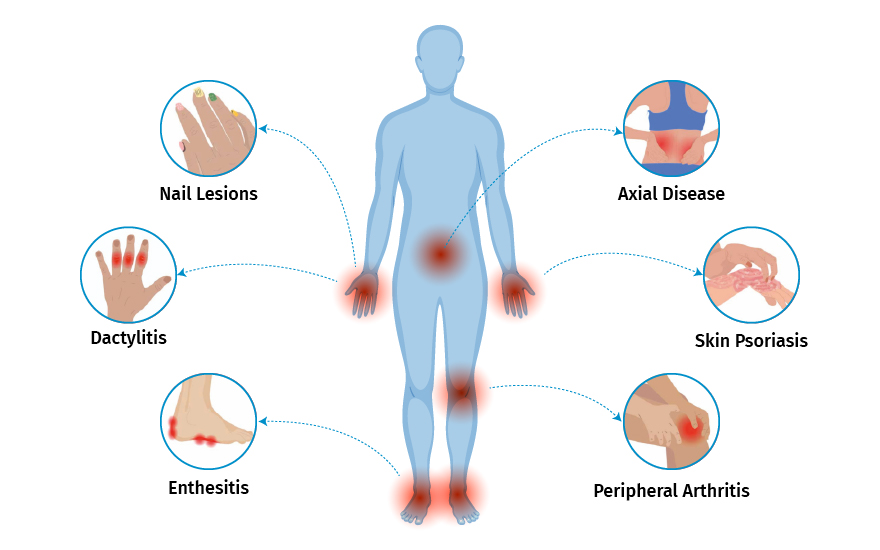
PsA does not follow a single pattern and can affect different joints in different ways. The common forms include

This form mainly affects the small joints closest to the nails on fingers and toes. Nail changes such as pitting, ridges, or discoloration often accompany joint inflammation.

Similar in appearance to rheumatoid arthritis, this type involves five or more joints on both sides of the body. It commonly affects the hands, wrists, and knees. Symmetry is key here, as the same joints on both sides are usually involved.

In this form, two to four joints are affected in an uneven pattern. One side of the body may have swollen joints while the other side remains unaffected. This is one of the most common forms of PsA.

This type affects the spine, sacroiliac joints, or neck. Patients may experience chronic back pain, stiffness, and reduced flexibility. Spondylitis can lead to postural changes if untreated.

A rare but severe form of PsA that causes bone erosion and joint deformity. It usually affects the small joints of hands and feet, leading to shortening or “telescoping” of fingers or toes.
The exact cause of PsA is not fully understood, but it involves a combination of genetic, immune, and environmental factors
PsA can affect joints, skin, nails, and even eyes. Symptoms may appear gradually or suddenly and often vary in severity.


PsA treatment focuses on relieving symptoms, controlling inflammation, and preventing joint damage.

Diagnosing PsA requires a careful combination of clinical evaluation, lab tests, and imaging:
