Enteropathic arthritis is a form of chronic, inflammatory arthritis associated with the occurrence of an inflammatory bowel disease (IBD), the two best-known types of which are ulcerative colitis and Crohn’s disease. About one in five people with Crohn’s or ulcerative colitis will develop enteropathic arthritis.
The most common areas affected by enteropathic arthritis are inflammation of the peripheral (limb) joints, as well as the abdominal pain and possibly bloody diarrhea associated with the IBD component of the disease. In some cases, the entire spine can become involved as well.
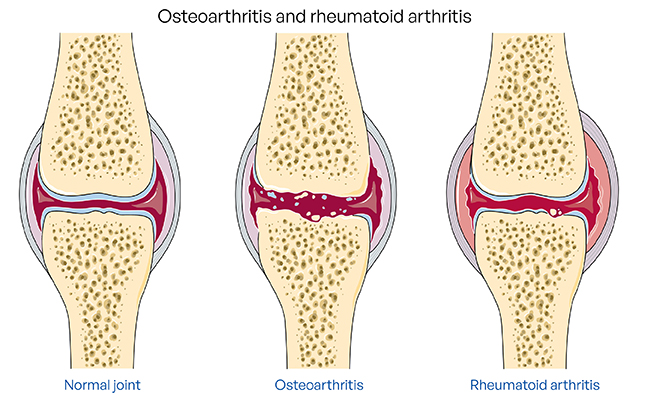
Recognizing joint, spine, and inflammation-related symptoms associated with enteropathic arthritis.




Key factors that contribute to the development of enteropathic arthritis.
Diagnosis is based on symptoms, medical history, and clinical findings, particularly the presence of inflammatory bowel disease (IBD).
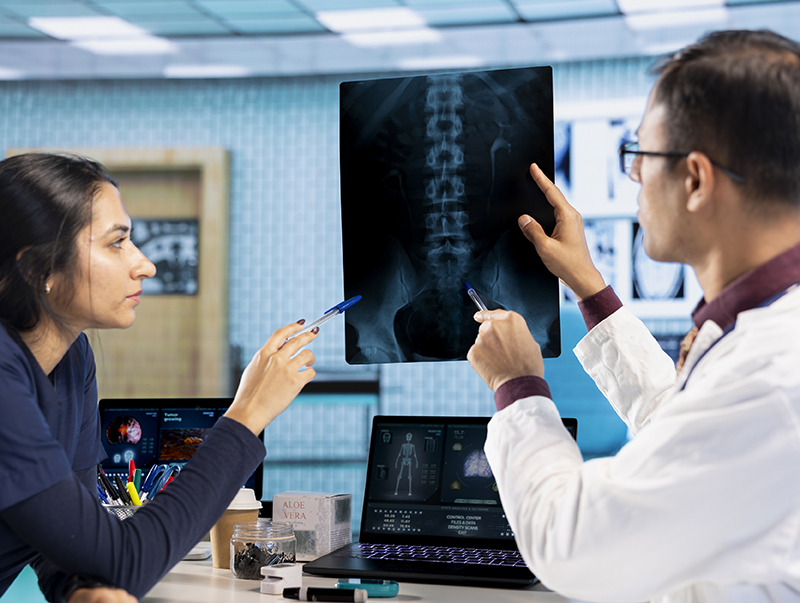
Personalized care strategies to control joint pain and support gut health.

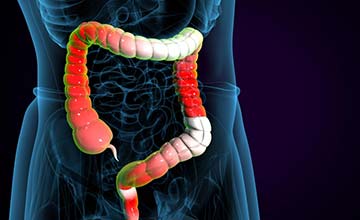



Managing daily life with enteropathic arthritis involves a multifaceted approach: