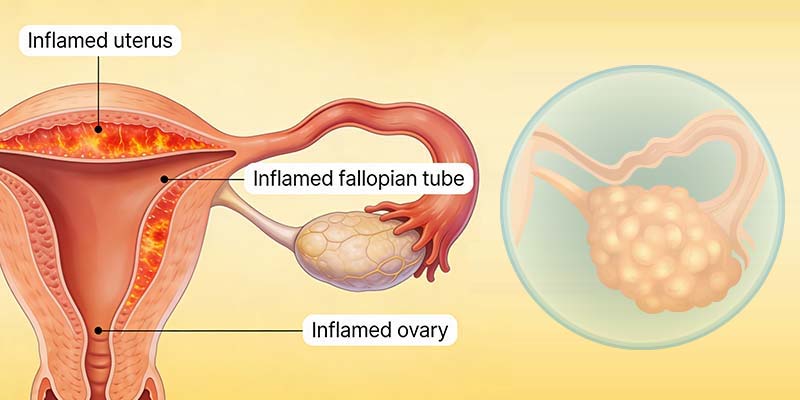
Systemic inflammation refers to a long-lasting inflammatory response that affects the entire body. While inflammation is a natural and necessary process that helps the body fight infections and heal injuries, problems arise when it becomes chronic. In women, persistent inflammation can interfere with hormonal balance, menstrual health, fertility, and pregnancy outcomes. Many reproductive health issues that women face today are now being linked to underlying inflammatory processes, making this an important topic for awareness and prevention.
Systemic inflammation occurs when the immune system remains continuously activated, even when there is no immediate threat. Instead of protecting the body, this ongoing inflammatory state begins to damage healthy tissues and organs. It is often influenced by lifestyle factors such as poor diet, stress, lack of physical activity, obesity, and long-standing medical conditions.
There are two main types of inflammation. Acute inflammation is short-term and beneficial, helping the body recover from injury or infection. Chronic inflammation, on the other hand, develops slowly and may persist for months or years without obvious symptoms. Over time, this silent inflammation can disrupt normal reproductive functions and increase the risk of hormonal and fertility-related problems.
The female reproductive system functions through a delicate balance between hormones and the immune system. Hormones such as estrogen and progesterone regulate ovulation, menstrual cycles, and pregnancy, while the immune system protects reproductive tissues and supports embryo implantation. For healthy reproduction, the immune response must be carefully controlled—not too weak and not overly active.
When systemic inflammation is present, this balance is disturbed. Hormonal signals may become irregular, ovulation can be affected, and the reproductive organs may not function optimally. This disruption can make it harder to conceive and maintain a healthy pregnancy.
Systemic inflammation can interfere with multiple stages of the reproductive process, from ovulation to implantation and pregnancy maintenance. When inflammation becomes chronic, it creates an unhealthy internal environment that affects reproductive organs and hormonal signaling.
Fallopian tube blockage can develop when long-term inflammation causes swelling, irritation, or scarring within the fallopian tubes. Over time, repeated inflammatory responses may lead to fibrosis, where normal tissue is replaced by scar tissue. This narrowing or blockage prevents the egg and sperm from meeting naturally, making conception difficult. In some cases, inflammation-related damage to the tubes increases the risk of ectopic pregnancy, where the fertilized egg implants outside the uterus, posing serious health risks.
Ovarian dysfunction is another major effect of persistent inflammation. Inflammatory chemicals released in the body can disrupt the normal development of ovarian follicles and interfere with ovulation. This may result in irregular or absent menstrual cycles and reduced egg quality. Poor egg quality not only lowers the chances of conception but also increases the risk of early pregnancy loss. Over time, inflammation can contribute to a decline in ovarian reserve, making fertility challenges more pronounced with age.
A healthy uterine environment is essential for the embryo to implant and grow. Systemic inflammation can reduce blood flow to the uterus and alter the structure and function of the uterine lining. When the endometrium is inflamed, it may become less receptive to embryo implantation. This can lead to implantation failure, early miscarriages, or repeated pregnancy losses. Even when fertilization occurs successfully, an inflamed uterine environment can make it difficult for pregnancy to continue.
Inflammation also affects fertility through immune system dysregulation and autoimmune disorders. When the immune system becomes overactive, it may mistakenly attack reproductive tissues or interfere with hormonal balance. This immune imbalance can prevent implantation, disrupt early pregnancy, or increase the risk of pregnancy complications. In autoimmune conditions, ongoing inflammation further increases stress on the reproductive system, affecting both fertility and maternal health.
Overall, systemic inflammation acts as a hidden barrier to reproductive health. By damaging reproductive organs, disrupting hormones, and altering immune responses, chronic inflammation can significantly reduce fertility and increase pregnancy-related risks. Early identification and proper management of inflammation are key to protecting reproductive function and improving outcomes.
Reducing systemic inflammation is an important step in improving fertility outcomes. Since inflammation can affect ovulation, implantation, and pregnancy maintenance, addressing its root causes can significantly enhance reproductive health. Every fertility journey is different, and treatment approaches should be personalized based on the underlying cause and severity of inflammation.
Medical management plays a key role in reducing inflammation when it is caused by infections, autoimmune responses, or structural issues within the reproductive system. Depending on the diagnosis, healthcare providers may recommend anti-inflammatory medications to reduce swelling and tissue irritation in the reproductive organs. In cases where chronic infection is present, antibiotics may be prescribed to eliminate the source of inflammation and prevent further damage.
When inflammation leads to scarring or blockages—such as in endometriosis or pelvic inflammatory disease—surgical intervention may be required. Surgery can help remove scar tissue, restore normal anatomy, and improve the chances of natural conception or assisted fertility treatments.
Diet plays a powerful role in controlling chronic inflammation. An anti-inflammatory diet supports hormonal balance and improves overall reproductive health. Consuming foods rich in antioxidants, healthy fats, and essential nutrients helps the body reduce inflammatory responses and repair tissues.
Foods that support reproductive health include:
In some cases, supplements such as omega-3 fatty acids, vitamin D, or curcumin may help reduce inflammation. However, supplementation should always be guided by a fertility specialist or healthcare provider to ensure safety and effectiveness.
Chronic stress can worsen inflammation by increasing stress hormones that disrupt immune and hormonal balance. Managing stress is therefore an essential part of improving fertility. Mind-body practices such as yoga, meditation, and controlled breathing help calm the nervous system and reduce inflammatory activity.
Healthy lifestyle habits also play a critical role. Regular physical activity, adequate sleep, avoiding smoking, limiting alcohol intake, and maintaining a healthy weight can significantly lower inflammation levels. These changes not only improve fertility outcomes but also support long-term reproductive and overall health.
When inflammation has caused significant fertility challenges, assisted reproductive technologies (ART) such as IVF or ICSI may be recommended. These treatments can help overcome barriers like blocked fallopian tubes, poor egg quality, or sperm-related issues caused by inflammation.
In women who experience repeated implantation failure due to an inflamed uterine environment, additional approaches such as immune-based therapies may be considered. These treatments aim to regulate immune responses and improve endometrial receptivity, increasing the chances of a successful pregnancy.
Several common health conditions are strongly linked to systemic inflammation and can significantly affect women’s reproductive health. When these conditions are not well managed, they can worsen hormonal imbalance, disrupt menstrual cycles, and reduce fertility. Understanding how each condition contributes to inflammation helps in taking early and effective action.
Polycystic Ovary Syndrome (PCOS) is one of the most common reproductive disorders associated with low-grade chronic inflammation. In women with PCOS, inflammatory substances in the body interfere with how insulin works, leading to insulin resistance. This, in turn, causes higher insulin levels, which stimulate excess androgen (male hormone) production. The hormonal imbalance affects ovulation, often resulting in irregular or missed periods and difficulty in conceiving. Over time, ongoing inflammation in PCOS can also increase the risk of metabolic issues such as type 2 diabetes and cardiovascular problems.
Endometriosis is a condition driven largely by inflammation, where tissue similar to the uterine lining grows outside the uterus. This misplaced tissue triggers an inflammatory response, causing chronic pelvic pain and the formation of scar tissue and adhesions. The inflammation can affect the ovaries, fallopian tubes, and uterus, making it harder for fertilization and implantation to occur. In many women, persistent inflammation from endometriosis contributes to reduced fertility and negatively impacts quality of life.
Autoimmune and metabolic disorders, such as rheumatoid arthritis, ankylosing spondylitis, and metabolic syndrome, also increase systemic inflammation. In autoimmune diseases, the immune system mistakenly attacks healthy tissues, keeping the body in a constant inflammatory state. This ongoing immune activity can interfere with hormone regulation and reproductive organ function. Metabolic disorders, especially those linked to insulin resistance, further worsen inflammation and may lead to irregular menstrual cycles, ovulatory dysfunction, and higher risks during pregnancy, including miscarriage and pregnancy complications.
Overweight and obesity play a major role in increasing systemic inflammation. Fat tissue is not just a storage organ; it actively releases inflammatory chemicals known as cytokines. These substances disrupt normal hormone signaling and interfere with ovulation. Excess weight can also worsen conditions like PCOS and insulin resistance, creating a cycle where inflammation and hormonal imbalance feed into each other. As a result, overweight and obese women may experience irregular periods, reduced fertility, and higher chances of pregnancy-related complications.
Because these conditions are interconnected through inflammation, certain factors require ongoing attention and management.
These include:
Managing systemic inflammation through lifestyle changes, medical treatment, and regular monitoring can greatly improve reproductive health outcomes and overall well-being.
Systemic inflammation is a hidden but powerful factor influencing women’s reproductive health. When left unmanaged, it can disrupt hormones, damage reproductive organs, and reduce fertility. The good news is that inflammation can often be controlled through timely medical care and healthy lifestyle choices.
By focusing on balanced nutrition, regular physical activity, stress management, and early treatment of underlying conditions, women can reduce inflammatory burden and support long-term reproductive health. Addressing systemic inflammation is not only essential for fertility but also for overall well-being throughout life.