In recent years, advances have been made in the treatment of ankylosing spondylitis and related diseases. There is a lot that can be done to relieve the pain and stiffness of AS. Recent studies show that the new biologic medications (TNF-α inhibitors) can potentially slow or halt the disease progression in some people.
A common treatment regimen involves medication, exercise and possibly physical therapy, good posture practices, and other treatment options such as applying heat/cold to help relax muscles and reduce joint pain. In severe cases of AS, surgery may also be an option. Very often, a rheumatologist will outline a treatment plan, but other professionals may also be able to help.
Treatment options guided by specialists to help you manage Ankylosing Spondylitis with confidence and control.
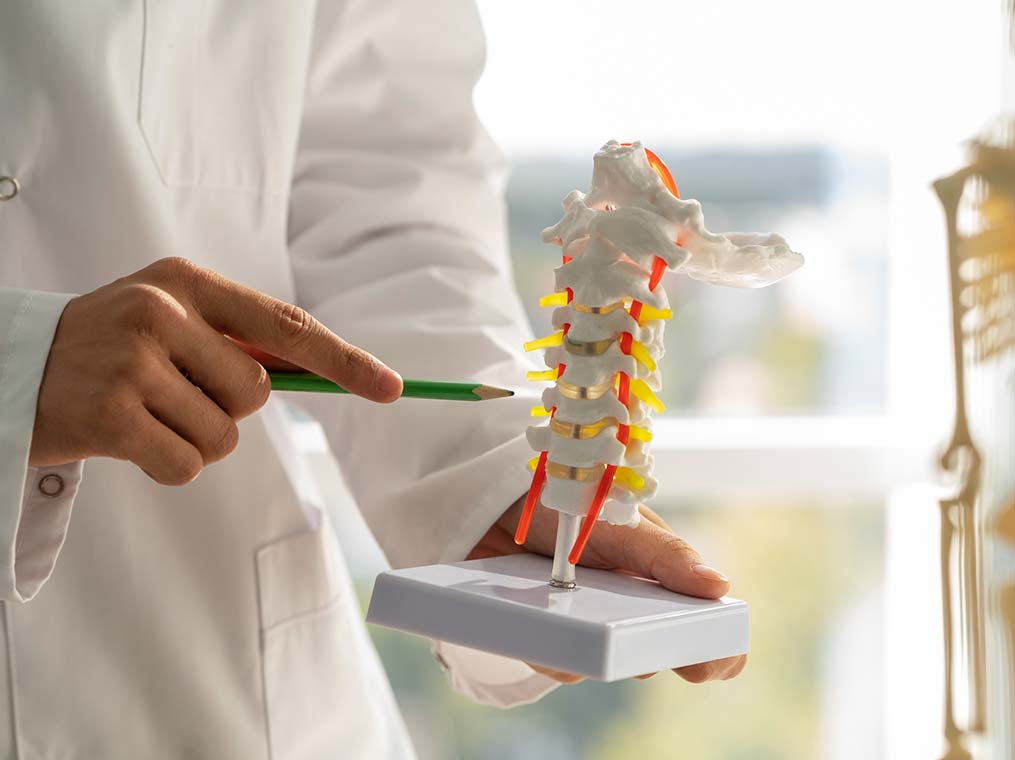
Medical treatment plays a central role in managing Ankylosing Spondylitis (AS). The primary goal is to control inflammation, relieve pain, maintain mobility, and prevent long-term joint and spinal damage. Because AS affects individuals differently, treatment plans are highly personalized and may evolve over time based on disease activity, symptom severity, and response to therapy.
A rheumatologist typically guides medical treatment, often combining medications with physical therapy and lifestyle adjustments for optimal outcomes.

NSAIDs are usually the first line of treatment for Ankylosing Spondylitis. These medications help reduce inflammation, ease pain, and improve stiffness, particularly morning stiffness that is common in AS.
Commonly prescribed NSAIDs include:
For many people with mild to moderate AS, NSAIDs alone may provide sufficient symptom relief. However, long-term or high-dose use requires careful monitoring, as NSAIDs can cause stomach irritation, kidney issues, or increased cardiovascular risk in some individuals.

DMARDs are used when Ankylosing Spondylitis affects peripheral joints, such as the hips, knees, shoulders, or ankles. While DMARDs are not highly effective for spinal inflammation, they can help manage joint-related symptoms and reduce inflammation outside the spine.
Common DMARDs used in AS include:
These medications work by modulating the immune system and may take several weeks or months to show noticeable benefits. Regular blood tests are usually required to monitor potential side effects.
Biologic medications represent a major advancement in the treatment of moderate to severe Ankylosing Spondylitis. These targeted therapies work by blocking specific inflammatory pathways involved in the disease process.
TNF inhibitors are commonly prescribed when symptoms are not adequately controlled with NSAIDs. They have been shown to significantly reduce pain, stiffness, and inflammation while improving physical function and quality of life.
Examples include:
IL-17 inhibitors are an option for individuals who do not respond well to TNF inhibitors or cannot tolerate them.
Examples include:
Biologics are administered via injections or intravenous infusions and require ongoing medical supervision to monitor infection risk and overall immune health.

Corticosteroids are sometimes used for short-term symptom control during disease flare-ups. They may be given as:
Common DMARDs used in AS include:
Due to potential side effects, corticosteroids are not recommended for long-term management of Ankylosing Spondylitis.
In some cases, additional medications may be prescribed to help manage symptoms, such as:
These treatments focus on symptom relief rather than disease control and are usually used alongside core therapies.


Ankylosing Spondylitis is a chronic condition, and treatment needs may change over time. Regular follow-ups allow healthcare providers to:
A proactive, long-term treatment strategy helps maintain mobility, reduce complications, and support overall quality of life.
Incorporating healthy habits into daily life can greatly improve symptom control and slow disease progression.

Maintaining proper posture while sitting, standing, and sleeping helps prevent spinal deformity and stiffness.


Smoking worsens inflammation, reduces lung capacity, and accelerates disease progression. Quitting smoking is one of the most impactful lifestyle changes for AS patients.

Although no specific diet cures AS, maintaining a balanced diet and healthy weight reduces strain on joints and supports overall immune health.
At Antardhwani, we believe in a holistic, patient-first approach to Ankylosing Spondylitis care. We help individuals by providing:
Our mission is to empower people living with AS to make informed decisions and feel supported at every stage of their journey.
What’s new in our journey against arthritis and spondylitis.